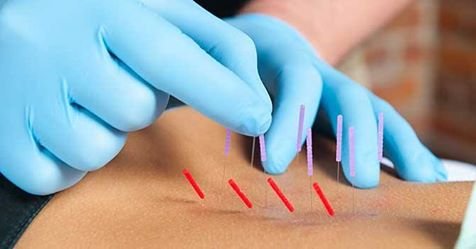
Troy Tribble, 41, swung to “dry needling” to move his back agony and fits.
He’s had a few sessions. Each time his physical specialist deals with an alternate territory. For Tribble, of Suwanee, it has improved things greatly.
The change he has encountered is “in my agony level and how every now and again the fits come,” Tribble says. It has helped him recover the personal satisfaction he used to have, he includes.
“If it’s all the same to you a little needle pricking,” it’s an advantageous treatment, he says. “Contrasted with the torment that I was in, [the needle prick] didn’t make a difference.”
Dry needling utilizes a fine (filiform) needle intended to go into delicate muscle spots to mitigate torment and enhance muscle proficiency. The needle is at times portrayed as being more slender than the measurement of a feline’s hair.
The dry needling strategy does not (and can’t) infuse solution, as the needle has no opening for that reason — thus, the word dry. It’s commonly done via prepared physical specialists.
Versus Needle Therapy
Dry needling and needle therapy both utilize the filiform needle, however generally are extensively extraordinary.
With needle therapy, a mending system that grew over 2,000 years back in China, needles are put into exact focuses along particular pathways called meridians and are left there for a time frame amid the treatment.
With dry needling, a patient will point to an agonizing range. The physical specialist will embed a needle, at that point expel it (without the needle maintenance utilized as a part of needle therapy). The motivation behind every inclusion is to achieve a trigger guide, causing a muscle toward jerk.
As a method for treating torment, needling has pulled in developing enthusiasm for the United States (and some different nations) in the course of recent years.
As indicated by the American Physical Therapy Association, the execution of present-day dry needling by physical advisors depends on neuroanatomy (the sensory system) and current logical investigation of the apprehensive and musculoskeletal frameworks (how muscles and bones cooperate).
Valuable Chemicals
Needling accomplishes torment help through the arrival of endorphins and serum cortisol and makes an adjustment in the body’s vitality levels, says The Dry Needling Institute.
The organization says setting needles in the muscle’s trigger focuses brings about “confined draining, which advances recuperating by animating collagen and protein development.”
“The underlying fit that it makes feels extremely odd,” says Tribble, “however it leaves similarly as quick as it goes ahead.” It feels as though you have gone to the rec center and worked for muscle bunches you aren’t accustomed to working, he says.
Nehama Schondorf, a physical specialist with Emory Rehabilitation Outpatient Center in Dunwoody, says dry needling can diminish nearby or “alluded” solid torment, enhance the scope of movement and help enhance quality.
Patients will take a stab at needling in the event that they can recapture their scope of movement in a joint — in any event to some degree if not totally.
Schondorf reviews one patient with a “solidified” shoulder who had taken a stab at everything from steroid infusions to general exercise-based recuperation with no alleviation. For her, a few sessions with needling prompted a genuine change.
“She was astonished by the change,” said Schondorf.
Trigger Focuses
Joseph Donnelly, the leader of the Physical Therapy Association of Georgia, says, “In the event that you have a myofascial trigger point inside a muscle that feels like a bunch, or there is a tight range in the muscle — it harms.”
Donnelly fills in as a clinical partner teacher at Mercer University’s Atlanta grounds.
“The part that damages the patient is really a contracture,” says Donnelly. “Patients point to where it harms. Obviously, the names they use to depict the torment are differed, in view of their uneasiness. Myofascial torment is likely not one of them.”
The patient can more often than not guide the PT to a sore spot. At that point, Donnelly clarifies, the PT enables the filiform needle to enter the trigger point (inside the muscle) to get the coveted jerk reaction.
This reaction can diminish torment created from the muscle, enhance muscle proficiency, and abatement compressive stacking over the included joint — particularly if the patient has encountered some degeneration.
There have been some expert turf fights between promoters of needle therapy and supporters of dry needling. This sort of contention is tragic, Donnelly says. The two sorts of treatment “are both great, and each has its place.”
What Donnelly proposes is that acupuncturists and physical specialists consider what is best for the patient’s condition.
“Simply make persistent care first,” he says.
Symptoms
Physiatrists — doctors prepared in physical drug and restoration — concentrate on non-surgical strategies to re-establish ideal capacity. They are authorized to control “trigger point infusions,” a classification that consolidates infusing prescription and also needling.
“Dry needling can be difficult,” says Michael McHenry, a physiatrist at OrthoAtlanta. “Physiatrists can utilize prescriptions to influence the needling to process less difficult, and different meds that can give help over a more extended span.”
Truth be told, the physiatrist may join dry needling into a bigger treatment get ready for the patient being served by the active recuperation group.
“It is not a positive fix,” said Donnelly, when alluding to the system. “Patients need to take part in the remedial procedure, as well.” That implies remaining consistent with their prescribed home exercise program, particularly with regards to retraining for the pose.
Dry needling can be utilized as a feature of complex treatment for ceaseless musculoskeletal agony and can be connected by physiatrists, family doctors, rheumatologists, orthopedic specialists, torment authorities, dental practitioners, and physical advisors, as indicated by the APTA.
Each state commands what is permitted inside a well-being expert’s extent of training. With regards to dry needling, states’ guidelines fluctuate generally.
In Georgia, a generally qualified proficient requires an extra 50 hours of preparing to perform needling treatment.
Judi Kanne, an enlisted attendant, and independent essayist consolidate her nursing and news coverage foundations to expound on general well-being.